News + Ideas
MIG News
On April 4, the Downtown Boulder Vision Plan was awarded a Colorado Downtown Excellence Award for Best Partnerships in a Large Community.
MIG News
The WTS Portland Chapter selected TriMet’s Regional TOD Plan as its 2023 Innovative Transportation Solutions Award Winner.
MIG News
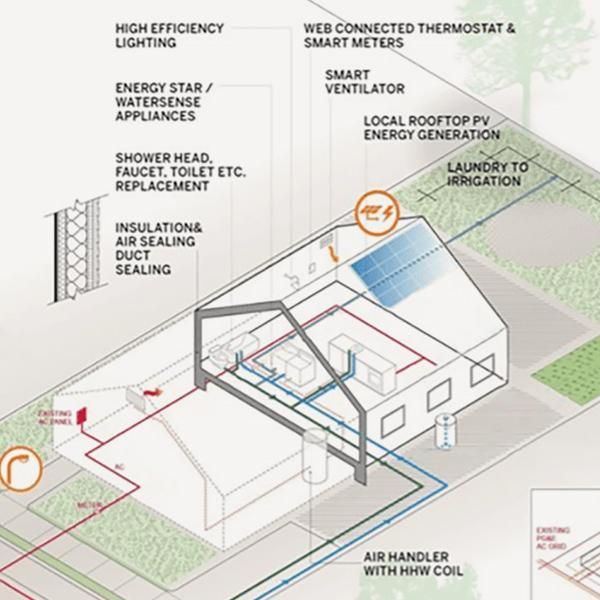
A bold approach to increasing energy efficiency and switching to renewable fuels is taking place in Oakland. EcoBlock. And MIG is helping create the template.
MIG News
The merger will deepen and expand sustainable landscape architecture and urban design services for clients in the Pacific Northwest.
Thought Leader
“We are in an Indigenous Renaissance…but there are still many circles of harm to break.” José de Jesus Leal, Director of MIG’s Native Nation Building Studio, shared his powerful perspective about Indigenous people and land at the recent National ASLA Conference in Minneapolis.
MIG News
She received one of ASLA’s highest honors, at the national ASLA meeting in Minneapolis.
MIG News
The Jury said: “This effort (Charlotte Future 2040) pushes planning in a new direction. The replicable ‘Place Type’ process can be a model for how to think about place more holistically and at a larger scale in other communities.”
Case Studies
Two corridors, both in a Vision Zero High Injury Network, now have community-based plans to improve safety and mobility, critical to the area’s economic development.
Case Studies
MIG's Houston Resilient Sidewalks Plan was recently awarded a 2023 Planning Achievement - Gold Award in Resilience from the Texas chapter of the American Planning Association.
MIG News
MIG's Houston Resilient Sidewalks Plan was recently awarded a 2023 Planning Achievement - Gold Award in Resilience from the Texas chapter of the American Planning Association.
MIG News
José de Jesus Leal will share innovative ideas about Indigenous ecological knowledge and how that can dramatically change our approach to climate action.
Case Studies
The US has had a fraught history in educating Native American children. “Growing Ute Futures” can profoundly change the future for the children of the Ute Mountain Ute Tribe.
MIG News
Even before the Plan is complete, its community engagement is recognized as a model for excellence—including innovative techniques for reaching people who have not traditionally engaged in land use planning.
MIG News
A new community park in Hillsboro, OR opened this month, featuring Oro, the friendly giant. It’s the area’s first and only purpose-built accessible park—its theme is: “woods gone wild.”
MIG News
A collaboration of 13 agencies, nonprofits and tribes will complete a 200-mile trail through the Olympic Peninsula.
MIG News
Article details how the Park Needs Assessment Plus project used data, including fitness trackers and smart phone apps, to increase park equity—as awards lauding the project come in.
Thought Leader
When we plan for climate change, we often think that scaring people will spur action. Turns out, that can freeze people. Jenni Zell, MIG’s Director of Regenerative Design, tells a story of how to thaw with hope.
MIG News
Fostering equity and youth development by providing a model for guiding investments in sports fields.
MIG News
A new hard-hitting and emotional campaign to reduce deaths from traffic crashes is launching in San José, California. It’s part of Vision Zero, an international effort to reduce traffic deaths to zero.
MIG News
As it turns 100, the company that provides water to the entire SF East Bay asked us to help it celebrate. Big time!
Case Studies
San Diego County is engaging the community in small actions that will make a big difference in its critical coastal waters.
Case Studies
A small coastal town turned to an old game to engage its community in new solutions.
MIG News
County Supervisors approved a data-driven plan to conserve 30% of land and coastal waters by 2030, advance park equity, and restore degraded land, especially in low-income communities.
MIG News
A once forlorn park will now reconnect the City with its River and revitalize the downtown.
MIG News
MIG’s new Downtown Brooklyn office—co-located with W Architecture and Landscape Architecture—now allows both firms to collectively push the boundaries of innovative, community-based solutions from coast to coast.
Thought Leader
New tradition-shattering campus planning models merge multiple academic levels, research and manufacturing—the results astound.
MIG News
How do you bring riders back to transit after a pandemic? A fresh take on an iconic brand promotes Muni transit service improvements for riders across San Francisco neighborhoods.
Thought Leader
Visualization tools let people “see” your planned project before it’s built—turning your community engagement on its head. And like with all technology, the costs might be less than you think.
Thought Leader
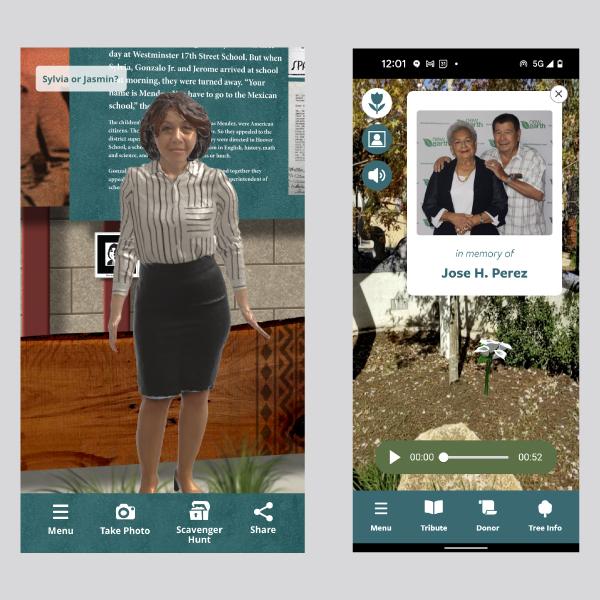
Parks are using new technologies to engage with and provide another experiential layer for visitors. It’s educational, it’s fun—and you don’t need to tell kids to put their phones away!
MIG News
The merger will deepen and expand services for clients in the Pacific Northwest. MIG | APG, will provide a full range of service, from planning and design to zoning and development codes, for both public and private sector clients.
Thought Leader
We need a new way to measure the “success” of urban planning. We can rethink planning to integrate equity, diversity and inclusion and address the unintended consequences of gentrification. MIG Principal Jay Renkens presented Charlotte North Carolina’s monumental shift in planning.
MIG News
A new park and park plan in Westminster promotes racial equity and honors local civil rights leaders.
MIG News
Earvin “Magic” Johnson Park is Project of the Year at the Sustainable Innovation Awards. And Santa Monica City Hall East won an award for zero waste.
MIG News
Two of 2021’s top websites for urban planning: Burlingame for its easy-to-use, highly informative digital plan and community process; Charlotte for its Virtual Open House
Thought Leader
How can cities plan future growth that’s equitable and thriving? MIG Principal Chris Beynon shares his experience—and plans for Kansas City.
MIG News
Jamillah Jordan, leader of MIG's Equity Studio, has been selected for the Robert Wood Johnson Foundation’s Culture of Health Leaders program.
Case Studies
California is rethinking building and transportation—aiming to drive less and protect the environment. SB743 is one of the “hottest” pieces of legislation to come out of Sacramento in quite a while.
MIG News
Recent wildfires impact park conservation, equity and health—and point to a need to plan for future extremes
MIG News
New York Aquarium’s “Ocean Wonders: Sharks” exhibit highlighted as part of ASLA’s Tools for Teachers program.
MIG News
We will not be silent. We will not look away. We will stand together.
MIG stands in solidarity with the Movement for Black Lives. We condemn racism, white supremacy and violence in all its forms. We commit to the active pursuit of racial equity.
MIG News
With Phase 1 already underway at the 120-acre Earvin “Magic” Johnson Recreation Area, the County approved funding to bring the AHBE | MIG masterplan closer to reality.
MIG News
Few things are as remarkable as the power of the human condition to both shape and be shaped by the world around us.
MIG News
The new play area for 3rd-5th grade students merges elements of Hong Kong's traditional culture with exciting climbing play, and won an OPAL award for interior design.
MIG News
“Easily read and clearly explained and illustrated, the book should be in the library of every municipal planning department, urban design firm, landscape architecture offices and community organizations promoting healthy living and great human spaces,” the EDRA jury stated.
MIG News
Landscape Architecture Foundation released its case study of Yanaguana Garden Play Area in San Antonio, citing quantifiable environmental, social and economic benefits.
MIG News
The new plan defines the essence of this Ashland park and won the Award of Excellence for Analysis & Planning from the Oregon ASLA.
MIG News
Should public agency workspaces look spartan and cost-effective so no one gets upset about wasting public money? The opposite, said MIG Principal Gary Lai in a think tank discussion.
MIG News
In uncovering centuries of history, the report balanced stories from multiple and often conflicting perspectives, posing the critical question: Whose narrative is it?
MIG News
This just in! A wealth of independent data, analysis and feedback that we often wish for and rarely get—Seattle’s Hing Hay Park is now a proven success.
MIG News
The City’s new Parks and Recreation Master Plan was recognized for innovative techniques and funding solutions, among other attributes.
MIG News
A cookie cutter is great for making a lot of equal cookies. But not for providing equitable parks for diverse communities. MIG has some better ideas and Park&Rec magazine features them.
MIG News
The Downtown Achievement Pinnacle Award recognizes the most creative and inspiring innovations in urban place management.
MIG News
MIG’s landscape architecture team in Portland has won Oregon ASLA’s 2019 Outstanding Firm Award, recognizing design excellence.
MIG News
Ocean Wonders: Sharks! at the New York Aquarium received a Top Honors Award from the Association of Zoos and Aquariums (AZA).
MIG News
The Summer 2019 California Park and Recreation Society magazine includes an article by MIG’s Cindy Mendoza and Lauren Schmitt about the new park standard: within a 10-minute walk.
MIG News
From Wendy Landman, ED of Walk Boston: “A terrific how-to manual for community activists and municipal staff…to bring streets back to life.”
MIG News
MIG Principal Melissa Erikson contributed to first-ever set of international guidelines that consider a broad range of abilities for designing the public realm.
MIG News
In this month’s “Landscape Architecture Magazine,” MIG Director of Landscape Architecture Brice Maryman shares an emerging set of “better practices.”
MIG News
“This book will be of great value to anyone who ever deals with streets in any capacity.”
MIG News
Seattle Neighborhood Greenways (SNG) has awarded its inaugural Community Enhancer Award to the newly redesigned Hing Hay park.
MIG News
“Making the world a better place” binds the two firms together.
Thought Leader
How can you create inclusive communities that lift children out of poverty? MIG Equity Studio Director Jamillah Jordan offers insights and catalytic solutions during her recent IDA Master Talk.
Thought Leader
Can your town or city—whether urban or rural, built-out or still developing, park-rich or park-poor—offer all residents the benefits of a park or recreation activity with a 10-minute walk? Absolutely. With a little imagination, collaboration and a fresh new perspective, every city can find opportunities to better connect people to parks.
MIG News
The accessible and sustainable beachfront playground in Santa Monica won 2019 Westside Urban Forum Design Award for Public/Open Space for AHBE | MIG.
MIG News
A new memorial will honor those lost in a tragic, massive mudslide near Oso Washington, as well as those who survived and the first and community responders.
MIG News
The MIG competition proposal won both the Conservation Innovation award and the coveted People’s Choice award for re-envisioning the Jordan River Parkway in Salt Lake County.
MIG News
An APA-award-winning project in Utah breaks new urban planning ground with virtual reality.
MIG News
The project, in Golden, Colorado, was one of only 16 projects nationwide to receive a Grand Award from the ACEC. All it took was a little magic.
Thought Leader
We’ve designed poor people out of our cities. Ideas for more inclusive designing.
MIG News
AHBE Landscape Architects joined urban planning and design firm, MIG, Inc., in 2019, creating MIG’s Los Angeles office.
MIG News
The Landscape Architecture Foundation funds studies to quantify why some environments perform better and offer more benefits than others. Yanaguana is one of them.
Thought Leader
MIG Principal Mukul Malhotra stunned the room with passion and poetry at the IDA conference in San Antonio. He spoke about how great cities and great buildings tell the story of place.
Thought Leader
Let’s go the next step beyond travel lanes and bike lanes, sidewalks and crosswalks. Let’s design streets for living, not just driving. Read Part 3 in the series of excerpts from our new book on inclusive design for the public realm.
MIG News
New immersive and interactive technologies will bring the U.S. Submarine Force—the “Silent Service”—to life.
MIG News
With new CEQA rules, you can take advantage of new opportunities to make better places with more choices for people and reduce the impact on the natural environment.
Thought Leader
Let’s go the next step beyond travel lanes and bike lanes, sidewalks and crosswalks. Let’s design streets for living, not just driving. Read Part 2 in the series of excerpts from our new book on inclusive design for the public realm.
Thought Leader
Let’s go the next step beyond travel lanes and bike lanes, sidewalks and crosswalks. Let’s design streets for living, not just driving. Excerpts from our new book on inclusive design for the public realm.
MIG News
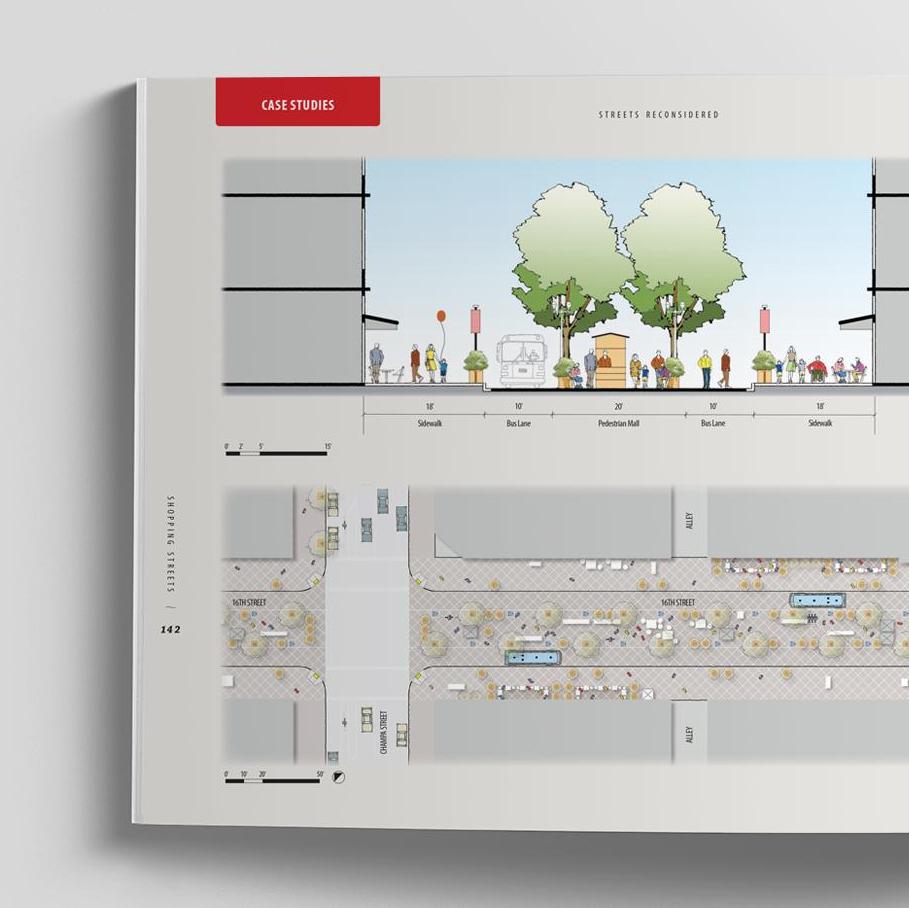
Streets Reconsidered: Inclusive Design for the Pubic Realm, by Daniel Iacofano and Mukul Malhotra, shows what streets can offer communities if they are designed for people, along with vehicles. Get a 20% discount!
Thought Leader
What are the next urban trends and transformations? MIG Principal Chris Beynon lays out 10 interconnected, disruptive and exciting mash ups you need to know about.
MIG News
Our innovative, weird and amphibious outdoor seating (a bathtub) has won the People’s Choice Award in Portland’s Street Seat Competition. You have to see it to believe it.
Case Studies
Every year, about 4 million gallons of polluted runoff entered Puget Sound. The County’s innovative solution enhanced the green space and didn’t require any mechanical or electrical systems.
MIG News
A new “backyard” at the San José Children’s Discovery Museum brings the joys of nature and the freedom to get dirty to kids in an urban environment.
Case Studies
Global issues, local stories, real actions: How a zoo exhibition tackled climate change and increased its revenue.
MIG News
San Diego-based MJE Marketing and MIG are now MIG | MJE, greatly expanding our marketing, branding, design, advertising, public relations and outreach services in Southern California.
Thought Leader
Innovative grantmaking is helping communities make streets safer and more equitable.
Thought Leader
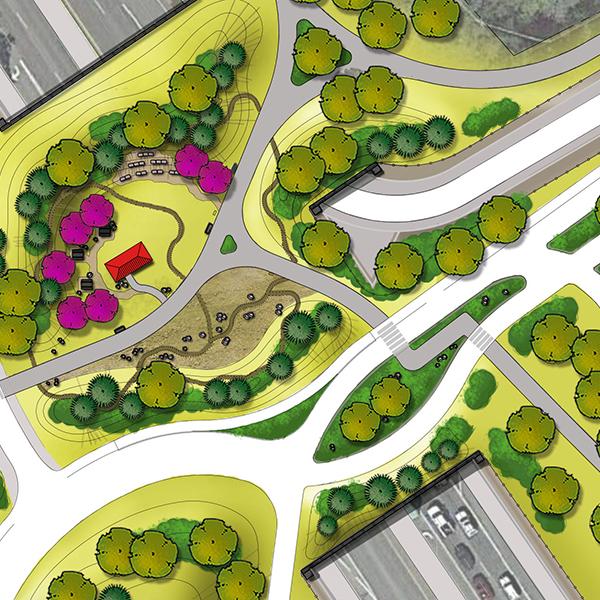
For communities with struggling commercial corridors and a lack of housing the plan for the City of Duarte’s new town center offers solutions.
Thought Leader
A MIG team interviewed homeless people in parks to better understand how park agencies can help them.
MIG News
MIG has created a partnership to launch a specialized web publishing platform...
MIG News
We are pleased to announce that The Portico Group (Portico) of Seattle, Washington, has joined MIG.
Thought Leader
MIG Principal Chris Beynon challenged communities and businesses to create inclusive cities that benefit all residents.
Case Studies
Three times as much parkland, bicycle and pedestrian connections to and through the park and to the River Walk, and a happy community.
MIG News
SvR brings an integrated approach to urban design that blurs the boundaries between landscape architecture, civil engineering, planning and applied ecology.
MIG News
We are pleased to announce that we have formed an alliance with Entitlement Advisors and Carol McDermott of Newport Beach, California.
MIG News
We are excited to announce that MIG | Portico Principal Alissa Rupp has been named a Fellow of the American Institute of Architects – AIA’s highest membership honor.
Thought Leader
For centuries thoughtful observers have recognized that play is integral to both childhood development and adult life.